Using cell mechanobiology to diagnose a rare gastrointestinal disease in infants and children
By LifETIME CDT Student: Sabah Sardar (University of Glasgow)
My PhD project focusses on a rare gastrointestinal disorder called Visceral myopathy (VSCM). This disease mainly affects infants and young children. However, in some cases it can develop in adulthood. VSCM is a pathological disorder of the intestinal smooth muscle cells where there is a problem with the contractile apparatus in the cells. This results in impaired intestinal function without any evidence of physical blockage in the intestines. VSCM patients can fall within a spectrum of disease severity ranging from problems with normal intestinal function to pseudo-obstructions affecting the intestines and bladder. Currently, treatment options are limited to complex and invasive procedures like catheterisation and surgical removal of the impaired intestine or total parenteral nutrition which is a feeding method that bypasses the gastrointestinal tract.
At present, there is no clear genetic marker that can be used for diagnosis of VSCM. This combined with the infrequency of the disease impacts early diagnosis and in turn affects treatment options available for patients. Ultimately, it can lead to potentially endangering interventions which need to be utilised to manage the disease. Therefore, it is essential to develop methods of early diagnosis to improve patient outcomes.
My project aims to identify label-free biomarkers for VSCM to improve early diagnosis of the disease. In order achieve this, I am screening for a set of valuable label-free biomarkers so that I can find one that best matches disease severity. I will be working in the cellular mechanobiology field which combines biology, physics and engineering to investigate cell function and behaviour. In my project, biomarkers will be identified based on non-specific physical indicators such as cell morphology (shape and height of cells), cell mechanics and the ability of cells to generate traction forces.
Currently I am investigating cell morphology using an optics-based method called ‘Dye Exclusion Microscopy’. This method enables the height of a cell to be measured by calculating the amount of light absorbed by a dye. The dye that is used needs to be a non-membrane permeable dye which means that it will not enter the cells but simple stay in the surrounding buffer. For dye exclusion microscopy experiments, visible light is passed through the sample. You can then calculate the absorbance of light by the dye in the presence and absence of cells. This allows you to determine the height of the cell and therefore gives you information on the cell shape. My hypothesis is that there will be statistically significant differences in cell height between healthy cells and VSCM cells. At the moment, I am optimising my protocol so that I can begin carrying out experiments on cell samples provided by VSCM patients. I am using the protocols published by (Schonbrun et al., 2013) and (Schonbrun et al., 2014) as the base and altering them to suit the cell type and the dye that I am working with.
Overall, the work I will carry out during my project will help in the diagnosis of VSCM. I hope to find a clear biomarker for the disease. This will allow further researchers to use my findings to develop innovative methods to carry out VSCM diagnosis in the clinical setting.
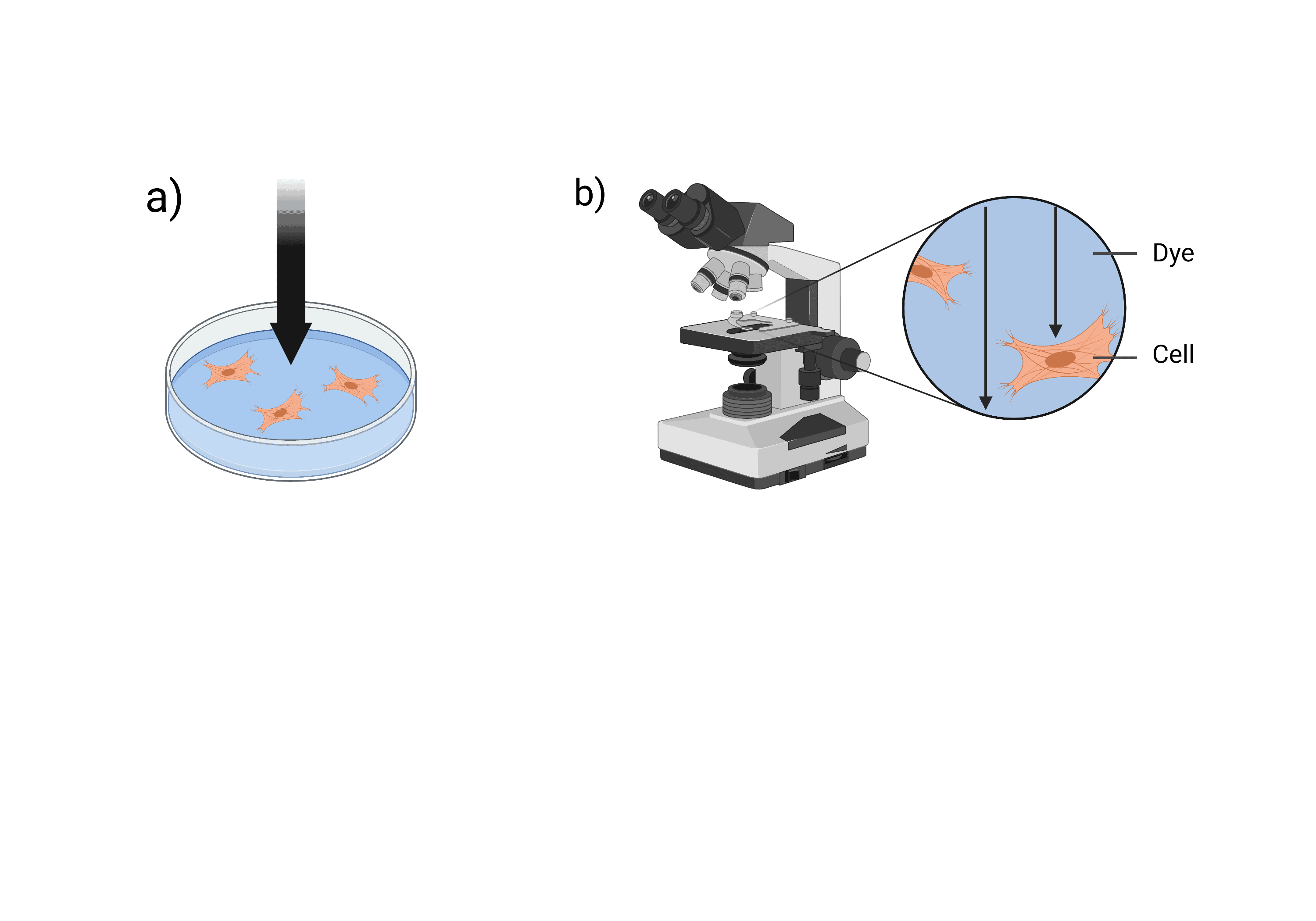
Figure 1: Outline of dye exclusion microscopy. Black arrows represent passage of light through the sample. a) shows light passing through the sample from above. b) shows a microscope analysing the sample as light passes through. Figure created with www.BioRender.com

Figure 2: Optimisation of dye exclusion microscopy protocol